Did you know that hypnotherapy is as effective as a low FODMAP diet for managing IBS? Crazy, right? Read on to find out more.
What is IBS?
Irritable Bowel Syndrome (IBS) is a functional condition. This means that the gut and body have no identifiable damage, and are essentially healthy. Yet, the gastrointestinal tract doesn’t appear to function as it should resulting in symptoms like bloating, wind, pain, constipation or diarrhoea. Although the exact cause of IBS is unknown, we do know that the connection between your gut and your brain (the gut-brain axis) plays an significant role.
What is the gut-brain axis?
If you’ve ever experienced butterflies in your stomach, then you’ve experienced the gut-brain axis in action. The head brain and the gut brain are connected by a two way super highway called the vagus nerve. The brain uses the vagus nerve to send messages to the stomach and intestines to control digestion. Meanwhile, the stomach and intestines send back information collected from the nerves in and around the gut. It’s thought that when you have IBS, your gut brain “over communicates” with the head brain and that some of these messages get scrambled. Sometimes messages will be in response to normal digestive processes (e.g. like your healthy gut bugs breaking down foods – called colonic fermentation) while at other times it may be in response to stress or heightened emotion. In the second case, it’s like that butterfly feeling is amplified as your body internalises the stress and emotion.
How is IBS managed?
There are three main ways of managing IBS; diet changes, medication, and psychological treatments. Given that IBS has multiple contributing factors that can affect symptoms, our experience at Everyday Nutrition is that people who get best results use a combination of therapies to target different parts of the puzzle. We call this your IBS toolbox:
- Low FODMAP diet limits certain carbohydrates that are fermented in the intestines creating gas and attracting water. Research shows that a low FODMAP diet helps about 75% of people with IBS achieve a significant and consistent improvement in abdominal symptoms.
- Medications like laxatives, antispasmodics and antidepressants can help manage symptoms. Although these appear to be less effective than modifying diet.
- Gut directed hypnotherapy which is believed to help reprogram the gut-brain axis and appears to be as effective as a low FODMAP diet
What is gut-directed hypnotherapy?
To understand how gut hypnotherapy works, we need to understand a bit more about how our gut communicates. Research shows that stress can interfere with the signals sent through the vagus nerve which can increase or decrease gut contractions, triggering IBS type symptoms. In addition, stress itself appears to alter the gut microbiome (this can change the balance of our healthy gut bacteria). It’s thought that this can lead to a constant state of “fight or flight” and keep our nervous system on continual alert for that sabre toothed tiger we might have to run away from.
It’s not known why people with IBS are more sensitive to gut stress, but we do know that they often have increased levels of the stress hormone, cortisol and they are more likely to have experienced physical or emotional trauma. In addition, we know that strong emotions, like anger, aggression and excitement can increase contractions along your intestines, while feelings of happiness can relax them.
Gut directed hypnotherapy involves guiding you into a relaxed state and then making new suggestions to your subconscious mind that are relevant to your symptoms. This helps to “reprogram” the gut-brain connection. During the session, you might be asked to imagine your gut as a free flowing river with no obstacles or blockages, everything working properly, or consuming an elixir that coats the gut and protects it, so that it works perfectly. Rest assured, that while under hypnosis, you are still able to talk, listen and think rationally.
The treatment usually involves 4-5 sessions with a psychologist who has specific training in gut directed hypnotherapy. During the sessions all you do is sit back with your eyes closed and listen, much like a guided meditation. At no point are you not in control. Sessions are often recorded so that you can listen to them at home, reinforcing the positive changes and teaching you self-hypnosis skills that you can draw on at any time.
What does the Research say?
In a 2016 Monash completed a study that compared the Low FODMAP diet against Gut Directed hypnotherapy (you can read the study here). They randomly separated 74 participants medically diagnosed with IBS into one of three groups; 1) low FODMAP diet with a FODMAP trained dietitian 2)gut directed hypnotherapy with a trained psychologist and 3) a combination of the two therapies.
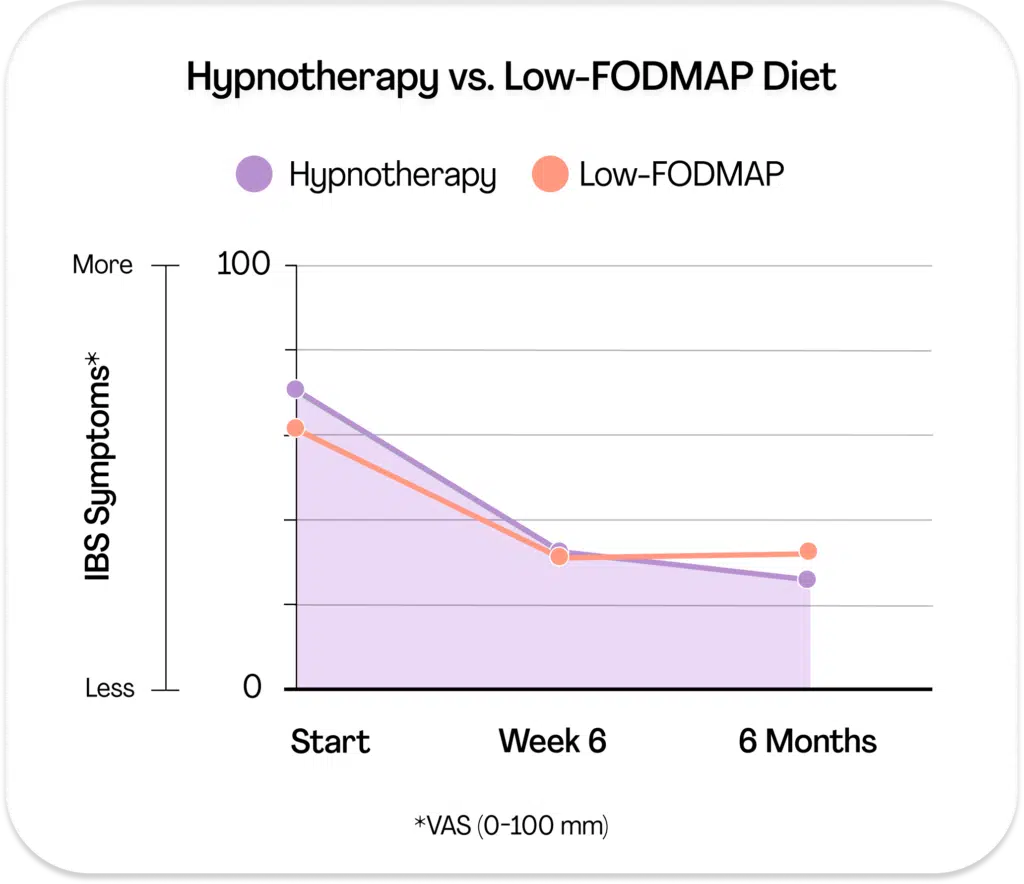
Participants were assessed at the start of the study, at the 6 week mark and again 6 months later for symptoms severity, quality of life and anxiety and depression. The good news is that, at the 6 week mark, all groups had achieved a significant and consistent improvement in gastrointestinal symptoms, with no significant difference between the groups. Even better, this improvement was maintained at the 6 month mark, leading researchers to conclude that gut directed hypnotherapy was as effective as the low FODMAP diet for managing IBS.
Where can you access hypnotherapy
If for some reason a low FODMAP diet isn’t for you or if you don’t get a result with it, you might like to consider trialling gut directed hypnotherapy. There are two main options for accessing gut directed hypnotherapy and which you choose will likely depend on your individual situation.
- Seeing a psychologist who has extra training in gut directed hypnotherapy and experience in managing IBS. A psychologist will assess your situation and develop hypnotherapy sessions to meet your specific needs. To find a psychologist, you might be able to get a recommendation from your doctor or visit the Australian Psychology Society website.
- You can now get gut directed hypnotherapy via an app called Nerva. Nerva is a 6 week program that involves listening to a 15 minute hypnosis each day. It’s based on the research completed by Monash University and only costs about as much as one individual session with a psychologist.
As I write this, I am three weeks into using Nerva and loving it. I’m also finding that I feel calmer and more relaxed all over, including in my gut.








3 Comments